S H Ho Urology and Laparoscopy Centre
Cutting Edge Urological Care with Compassion
Robotic Radical Prostatectomy
MBBS, FRCS, FICS, FAMS (Urology)
Senior Consultant & Board Certified Urologist (Singapore)
Gleneagles Medical Centre #09-18, Singapore 258499
Robotic surgery for prostate cancer




 Dr Ho Siew Hong
Make an appointment by email or call +65 64752512
Dr Ho Siew Hong
Make an appointment by email or call +65 64752512
Robotic assisted laparoscopic radical prostatectomy is a minimally invasive surgery to completely remove the prostate gland. It is
performed for men with early prostate cancer that is confined within the prostate and with a potential for cure.
The surgery is performed
by a urologist who controls the robotic arms. The urologist has total control of the robot at all times and at no stage is the surgery
automated.
Robotic radical prostatectomy is performed through several small holes in the abdominal wall. This allows access to the
prostate which is located deep in the pelvis. Through these small holes, surgical ports (or thin tubes) are inserted through which
specialized instruments are placed. These instruments are then controlled in a delicate fashion by the surgeon who sits at a console,
adjacent to the operating table.
A total of 6 small holes are made. At any one time the primary surgeon has control of four instruments which include the camera
and three surgical arms.
One of the significant advantages in robotic radical prostatectomy lies in the anastomosis or joint
between bladder and urethra. Accurate apposition between the bladder and urethra is made with the advantage of the flexibility of
the robotic arm in assisting the surgeon during surgical stitching. This results in lower incidence of urine leakage and better
urine continence after surgery.
The other advantage of the robotic radical prostatectomy lies in the better visualization of
the neurovascular bundle which allows for accurate dissection and preservation of the erection function nerves. This has resulted
in better erection function in patients where the nerves are spared during surgery.
The inherent advantages of minimal invasive surgery include shorter hospital stay, less post-operative pain, reduced convalescence
and a quicker return to normal activity. Patients are discharged with a catheter (a small plastic tube) in place which is usually
removed a week after surgery. An x-ray dye test called a cystogram, is performed prior to catheter removal confirm that the joint
has had knitted together before removing the catheter.
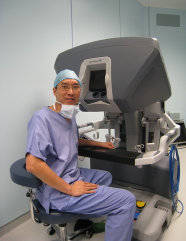
Dr Ho at the surgeon console
Cystogram x-ray test
Surgical wound a week later

Watch a video on Robotic Radical Prostatectomy by Dr Ho Siew Hong




 Dr Ho Siew Hong
Make an appointment by email or call +65 64752512
Dr Ho Siew Hong
Make an appointment by email or call +65 64752512
