If the varicocele is not causing any symptoms of pain and infertility is not an issue, no treatment is warranted. In cases of mild discomfort, the condition usually can be managed by wearing an athletic supporter or snug-fitting underwear during strenuous activity or exercise.
Treatment for varicocele is indicated in the following conditions:
a) Adolescent (age 12-18 years) with large varicocele and evidence of decreased testicular size.
The size of testes on the side where varicocele is present, is smaller than the opposite side.
Treatment is advised although the varicocele is not causing pain or other symptoms as it would improve function of the affected testes.
b) Any person with varicocele induced testicular pain.
Pain is usually described as 'dragging' and worse with prolonged exercise or standing.
c) Varicocele that is men who are subfertile or infertile
Correction of varicocele would result in 50%-70% improvement in men with low or poor sperm
count
Under general anaesthesia, three small incisions (5mm each) are made in the abdomen. Varicoceles on the right or left or both can be approached. The abnormal veins are identified and clipped and divided.
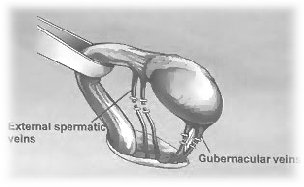
An x-ray dye is injected to map out where the problem is and where to embolize or block. By using coils or balloons, blood flow to the varicosed veins is blocked and is re-directed to other healthy pathways. The entire procedure can be completed within 2 hours.
Our centre prefers to reserve the embolization option for cases of varicocele recurrence after a surgical ligation.






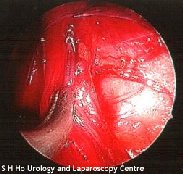
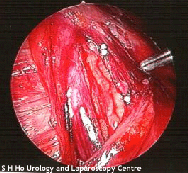







Advantages of laparoscopic varicocele surgery over other techniques include:
1. Accurate identification of all the veins and
avoiding injury to the artery and lymphatic vessels as the surgery is done under magnification during laparoscopy
2. Varicoceles
from both sides of the body can be corrected at the same time without needs for further surgical incisions
3. Rapid recovery
from surgery with minimal pain as the small 5mm wounds causes minimal trauma to tissue
Surgery is completed within 45 minutes,
even in the case of varicoceles occurring on both sides. Patient can be discharged a few hours after surgery and return to work is
within 48 to 72 hours.
Complications are rare. Injury to abdominal organs can occur in less than 1% of cases. Testicular artery
injury (1%) and hydrocele formation (1-5%) is not common. Improvement in sperm counts can be expected in 50%-70% of patients within
3 months. Overall pregnancy rates are between 10-20%.